 
It’s a long-term health burden for patients, the medical community - and the U.S. 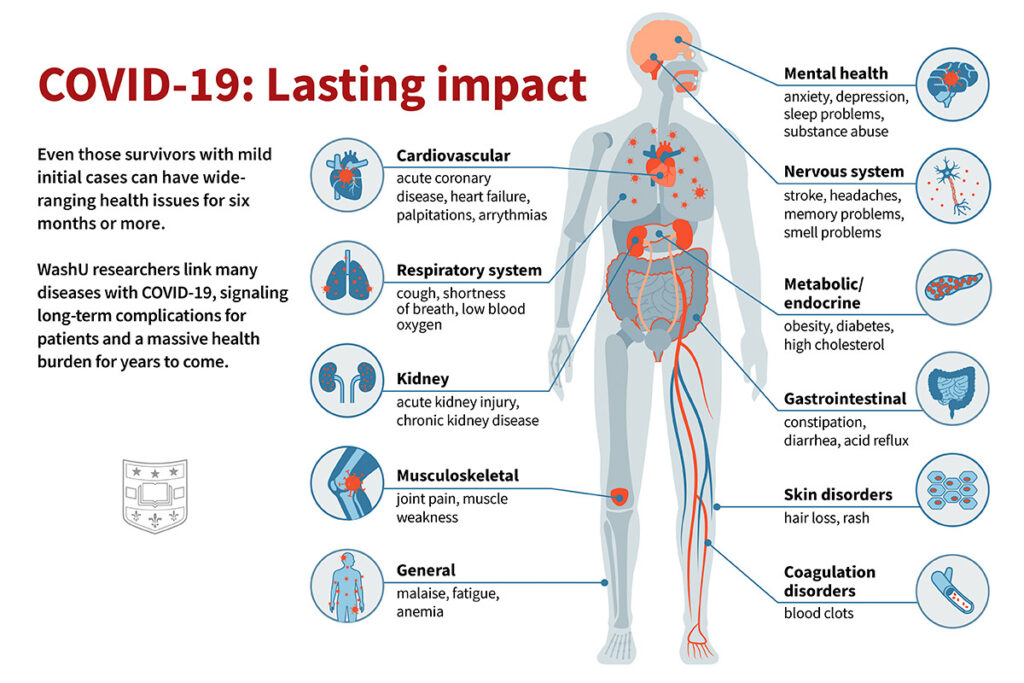
among those who recovered from the coronavirus.Since the start of the coronavirus pandemic we have seen the highest rate of kidney failure in our lifetimes. Steven Coca warns about the rise in “chronic kidney disease in the U.S. On this topic, Mount Sinai Health System Associate Professor of Nephrology and RenalytixAI Co-Founder, Dr. During July 2020, the impacts of COVID-19 on the kidneys made the news, following updated recommendations from the American Society of Nephrology. Kidneys: The American Society of Nephrology reported that approximately 50% of patients with severe cases of COVID-19 in intensive care experience kidney failure. Although rare, severe heart damage has also been seen in young, healthy people. Such heart damage might also explain long-term symptoms like shortness of breath, chest pain, and heart palpitations. In September, US CDC reported that heart conditions like myocarditis (inflammation of the heart muscle) and pericarditis (inflammation of the covering of the heart), are associated with COVID-19. In addition, heart problems have been reported in 40% of COVID-19 deaths. One German study reported that 78 out of 100 patients recovering from a COVID-19 infection had heart-related problems, such as inflammation and scarring, that could have serious consequences. Heart: Studies have shown that heart problems are also common. Early rehabilitation has been shown to improve respiratory (breathing) problems in patients who have had severe COVID-19. Lung problems may be short or long term, and experts have suggested that it can take months, possibly even more than a year, for lung function to return to normal after a COVID-19 infection. In any infected patient, COVID-19 may cause pneumonia (where the lungs fill with fluid), acute respiratory distress syndrome (ARDS), and sepsis (a bloodstream infection). Patients with lung problems like asthma, chronic obstructive pulmonary disease (COPD), and other chronic (long-term) lung diseases may be at higher risk of having complications from COVID-19. Lungs: Though it can impact other organs, COVID-19 is primarily thought of as a lung (or respiratory) illness. Recent studies document long-term impacts of COVID-19 on different organs in the body, including lung scarring, limited lung capacity, neurocognitive impacts, heart damage, renal failure, and more. The worse the symptoms of COVID-19 are, the more likely major organs are to be negatively impacted.ĬOVID-19 may impact organ systems directly (in the case of the virus causing inflammation in the lungs and airways) or indirectly (where organ damage is caused by illness that is a result of COVID-19 infection, but the organ damage is not caused by the virus infecting the organ directly). For more severe cases, short-term impacts may include respiratory (breathing) failure, confusion or other neurological problems, and kidney or heart damage due to a lack of oxygen or blood clots that can sometimes cause long-term problems. Many people infected with COVID-19 have mild or no symptoms, but some of the short-term impacts reported by people with mild symptoms include shortness of breath, fever, cough, fatigue (tiredness), and body aches.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
